A patient’s trust is won in the three minutes they spend navigating your interface. Since 70% of users expect healthcare to be as intuitive as a banking app, a clunky intake flow directly causes appointment abandonment.
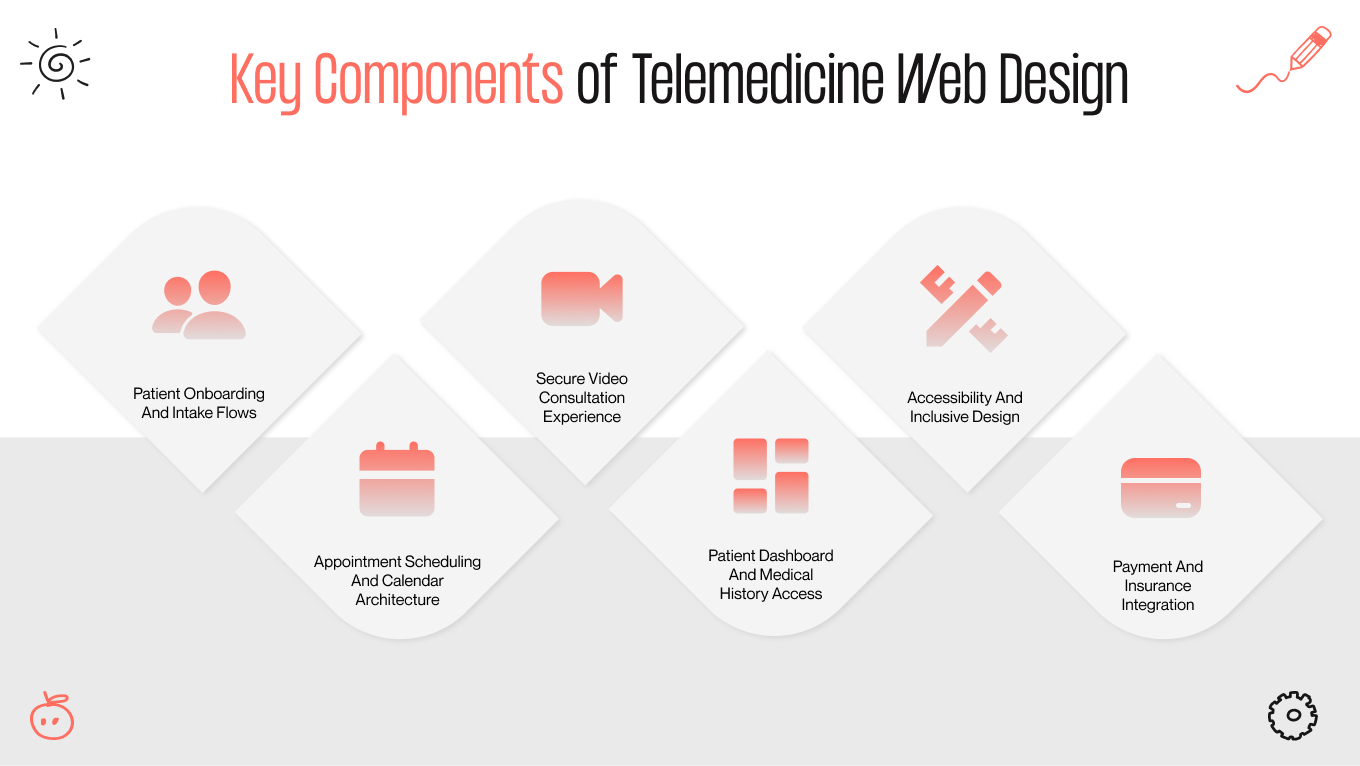
In telemedicine, design isn't surface. Scheduling, consent, authentication, and HIPAA compliance either work together as one coherent system or they don't work at all. When they don't, the damage is abandoned bookings, compliance exposure, and patients who chose someone else.
Our guide is built on a decade of Gapsy’s experience of healthcare platform design. It's a practical framework for founders who understand that the right decisions here improve the experience and determine whether the business scales.